A Participatory Design Methodology
The project is entirely designed through a participatory design methodology with each phase of the 6 phase model, to collect information from end-users. The following graphic is describing the methodology that is carried out through these phases.
The objective of the Tech labs was to verify that the technical components developed or made available by the technical partners were actually meeting the requirements previously validated. To achieve this result, the technical partners have developed a battery of tests. Each Technical lab tested an individualized set up in order to focus on specialized parts of the vCare system.
- Germany’s tech-lab performed extensive experiments for AI-based clinical pathway adaptation,
- Τhe technical site in Austria dealt with intelligent end-user interaction, and
- Spain’s site tested overall system integration
As a consequence, each Tech lab followed the concept of semi-integrated testing, where required vCare sub-systems were evaluated in terms of data flow and business logic. A semi-integrated test refers to an experiment for a particular sub-system, where data is partially simulated or collected offline to the extent that the sub-system can be confidently validated.
The Living Lab phase
The Living-Lab can also be described as a “physical space” that recreates the user’s usual living environment with the aim to observe the user’s interaction with technological solutions during the routine activities in real-life situations. For this trial, 80 patients are selected in four different clinical sites. The patients will be first trained to understand and use the solution by a multidisciplinary team composed of Physicians, Physiotherapists, Bioengineers, and Neuropsychologists operating inside the hospital and perfectly tuned with the system functioning.
Process
In fact, every patient, on the basis of his/her clinical needs and personal profile, is prescribed a number of activities. He then accomplishes a series of daily living scenarios defined in specific “Use Cases”. Those “Use Cases”, in the form of specific sessions, will be accomplished by every patient throughout 4 weeks. Each patient performs the sessions daily for 5 days each week.
Every session is monitored by a member of the clinical staff (medical doctor or physiotherapist). During the first two sessions, the clinical staff guides the interaction between the avatar and the patient. Then, the patients interact with the system features without assistance according to the planned test activities. The physiotherapist remains present in the room and observes the patient-avatar interaction in a non-intrusive way. In addition, the physiotherapist fills out a form in which he notes the adequateness of the patient-system interactions.
To make this whole process more understandable, the vCare partners created a great video that illustrates and explains the above process.
🎥 See the video here.
Focus on Parkison Patients
Parkinson is a slowly progressive disease, involving motor and nonmotor symptoms. All these symptoms impact patients’ quality of life.
The benefit and the use of vCare are that the patient is empowered to remain in control and is coached to avoid risks in everyday life, such as falling. At the same time, the patient improves functionality, autonomy, and quality of life. The vCare project can be used everywhere and helps all those who do not have easy access to traditional rehabilitation programs or when social distancing measures impose new specific constraints.
The Process
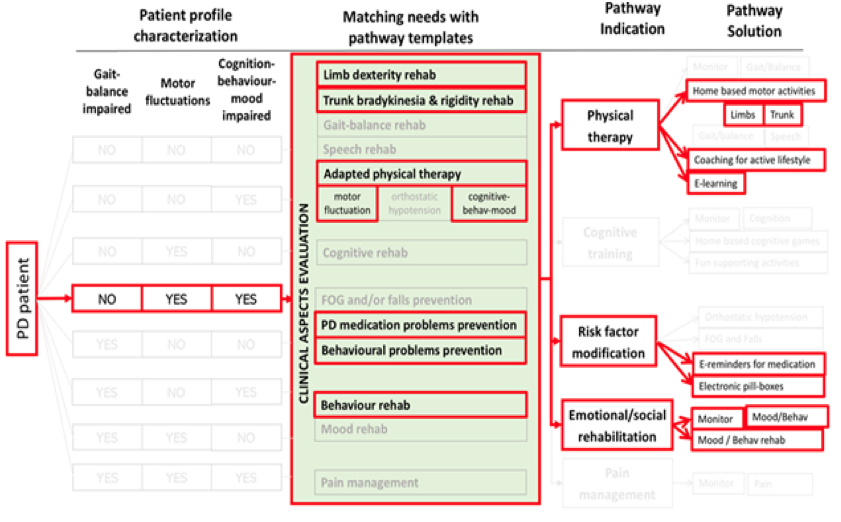
The patient basic profile is based on 3 main criteria. Once those have been specified, the system adapts the matching needs and the related pathway indications leading to the activation of a number of appropriate solutions. Those solutions can then be first further adapted by the clinician.
The patient is told to normally live his everyday routine life with the support of a Virtual Coach interpreted by an avatar that, interacting with the patient through a Tablet, will support him/her all day long along the rehabilitation sessions. Data coming from different sensors (e.g. environmental sensors to monitor the movements inside the house, “motion capture” systems to evaluate the execution of motor rehabilitation exercises) and provided by the patients and the caregivers are continuously processed to provide appropriate advice and feed-back to the patient. The clinical staff may at any time monitor the evolution of the situation of the patient.
The interactions with the virtual coach through the avatar displayed on the tablet can be very different: Arranging the best schedule for the rehabilitation sessions, giving precisions and feed-back about the exercises, advising about good lifestyle practices and/or alerting if the behaviour is not appropriate (e.g. too risky or too inactive) or promoting activities which trigger social interaction and virtuous behaviours.
Digital Therapeutics
Finally, the project stays close to innovation and developments and stands close to the Digital Therapeutic area. In November the project will participate on EHMA’s virtual conference by presenting the organisational consequences of the use of digital therapeutics such as vCare for the hospital. We look forward to seeing the next amazing steps and actions on this project!